What Are Varicose Veins: Causes, Symptoms, Treatments, and Prevention
Blood vessels, also known as veins, are tubes that move blood throughout every area of the body. While some essential veins are found deep inside the body, superficial veins are close to the skin. Depending on your skin tone, you might have some visible superficial veins, which is perfectly normal. But, what are varicose veins?
Most of the time, these superficial veins will look and function as they should. Their job is to move blood from the skin and surrounding tissues back into the deep vein system. Sometimes, however, superficial veins can become enlarged and highly visible beneath the skin, appearing rope-like and twisted. This is a condition known as varicose veins.
Varicose veins are not typically a major problem and shouldn’t be a cause for alarm. However, they can be uncomfortable or embarrassing and might make you feel self-conscious about your appearance. They can also lead to more serious health conditions in some cases, so it’s important to keep an eye on them once they develop.
This article will tell you how varicose veins develop and their symptoms, treatment, and prevention.
Varicose Vein Symptoms
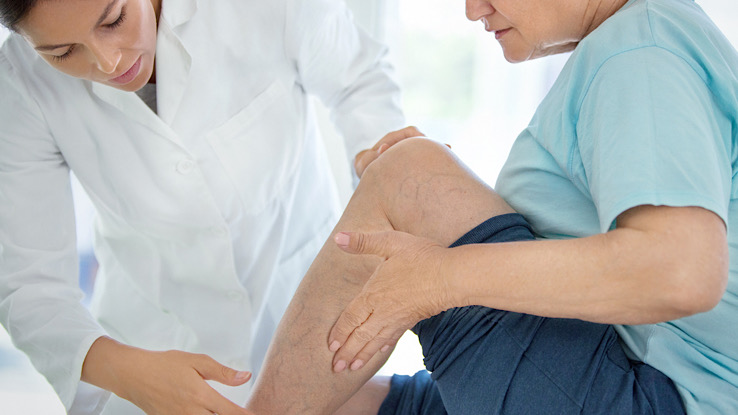
Varicose veins are usually easy to see. They appear as blue or purple bulges under the skin, most frequently occurring on the calves, ankles, and feet. Varicose veins can look like ropes or clumps beneath the skin.
Other varicose vein symptoms can include:
- Itchiness
- Swelling in the legs, feet, and ankles
- A heavy feeling in the legs
- Pain and aching
- Leg cramps
- Sores near the affected veins, known as venous ulcers
- Skin discoloration
Even when varicose veins aren’t painful, most people who develop them find their appearance upsetting. People with varicose veins often wear long pants at all times. They might avoid going to the beach or swimming pools, so they don’t have to feel self-conscious about the appearance of their legs.
Spider Veins vs. Varicose Veins
The terms “spider veins” and “varicose veins” are often used interchangeably, but they actually describe two different conditions. Both issues have to do with poor blood vessel function. However, spider veins are smaller, typically red in color, and do not bulge underneath the skin.
Unlike varicose veins, spider veins are unlikely to hurt and are solely a cosmetic issue. While they can be embarrassing, they’re not as large or noticeable as varicose veins. However, spider veins can occur on the face or legs, while varicose veins most often develop in the legs, ankles, and feet.
Causes of Varicose Veins
Varicose veins are caused by blood flow issues inside the blood vessels. Veins have valves that allow blood to flow through the blood vessels toward the heart. These valves also prevent blood from flowing backward.
If your veins have weak walls or damaged valves, then your blood will not flow efficiently, allowing it to pool up or travel backward, away from the heart. This can cause the veins to expand, bulge and twist. Increased blood pressure inside the veins from any source can also cause varicose veins.
Risk Factors for Varicose Veins
Females are much more likely to get varicose veins. It is thought that female hormones relax the blood vessel walls, making them more likely to weaken and become enlarged. Generally, the condition develops later in life, as veins start to deteriorate and lose their elasticity.
Other risk factors for varicose veins include:
- Genetics—if a close family member has varicose veins, you might get them too
- Pregnancy—increased blood volume during pregnancy can cause swollen veins
- Being overweight—extra weight increases pressure on the veins
- Being sedentary—sitting or standing for long intervals reduces blood flow
- Using tobacco products—nicotine damages blood vessels and can affect blood flow
Tips for Varicose Vein Prevention

It’s not always possible to prevent varicose veins from occurring, and some people will get them no matter what. Still, there are some tips you can follow to reduce the risk of developing varicose veins or to keep them from getting worse.
The best way to prevent varicose veins is to relieve pressure and promote circulation as much as possible. You want to keep the blood in your legs flowing toward your heart, so it doesn’t pool up in your veins. There are several steps you can take to promote healthy blood circulation:
- Exercise regularly—physical activity increases blood flow and promotes circulation
- Eat more fiber—fiber prevents constipation, which can cause more pressure on the veins
- Eat less salt—too much sodium can increase swelling
- Regulate your weight—losing weight can help relieve pressure on the veins
- Move frequently when standing—this helps promote blood flow and prevents blood from pooling
- Elevate your legs when sitting—to help blood flow toward the heart
- Wear compression socks—these socks fit over the calves and push blood up toward the heart, helping to prevent pooling
Diagnosing Varicose Veins
Diagnosing varicose veins is usually a simple process. Your doctor will perform an exam and check your legs while sitting and standing. They will ask about your lifestyle and family history to help confirm the diagnosis.
Your doctor might also recommend an ultrasound to examine your veins closely. If your doctor suspects you might have a blood clot, they might order a special kind of x-ray called a venogram. Imaging can help rule out other causes of your symptoms and give the doctor more information about the condition of your veins.
Treatments for Varicose Veins
Some people don’t need any treatment for varicose veins. Your doctor can recommend the best treatment option based on your symptoms.
If your varicose veins are mild, you might be able to keep them from getting worse with the preventative lifestyle changes outlined above. Your doctor might suggest pain management options if you’re experiencing discomfort, such as varicose vein cream to reduce pain in the affected area.
Treatments are available if your varicose veins are more severe or causing emotional and physical discomfort. These include:
- Sclerotherapy—a chemical injection procedure that seals off affected veins
- Endovenous ablation—a procedure that uses radiofrequency or laser therapy to seal varicose veins
- Surgery—removal of affected veins through a process called vein ligation or stripping
Although these procedures have some risks, they are fairly safe overall and require only a short recovery period. Your doctor should explain the risks and benefits before you decide on a treatment option.
If someone pregnant develops varicose veins, they will need to wait until they have given birth to consider treatment. Sometimes, the problem fixes itself after pregnancy as the body returns to normal.
It’s important to note that varicose veins can come back, even after treatment. If you develop new varicose veins after sealing off or removing other veins, you will need additional treatment to correct them.
Next Steps
If you’ve started to notice symptoms of varicose veins in your legs, it’s a good idea to check in with your doctor to get a confirmed diagnosis. Rarely, varicose veins can be associated with blood clots, and it’s important to have a doctor monitor your vein health. If you notice bleeding from varicose veins, call 911 right away.
Varicose veins are usually nothing to worry about, but they can be annoying and uncomfortable. Discuss your options with your doctor and consider taking steps to prevent your varicose veins from getting worse, whether you move forward with treatment or not.
Resource Links:
“Varicose Veins” via the Cleveland Clinic
“Varicose Veins” via the Mayo Clinic
“Varicose Veins and Spider Veins” via the Office on Women’s Health
“Varicose Veins” via the National Institute of Health





