Skin Conditions: Understanding Psoriasis Signs, Symptoms and Treatments

Psoriasis is a skin condition characterized most commonly by the appearance of dry, thickened skin patches. This chronic condition is not contagious, meaning it can’t be transmitted from one person to another. Scientists believe psoriasis is an autoimmune condition, which means it occurs due to a person’s overactive immune system attacking their body’s own healthy cells.
Psoriasis is generally diagnosed by a dermatologist (a doctor who specializes in skin conditions) because they can differentiate between this condition and others it may be commonly confused with, such as eczema. While there is no cure for this condition, people with psoriasis can manage their symptoms with a variety of treatment options. Keep reading to educate yourself about this condition.
Subtypes of Psoriasis
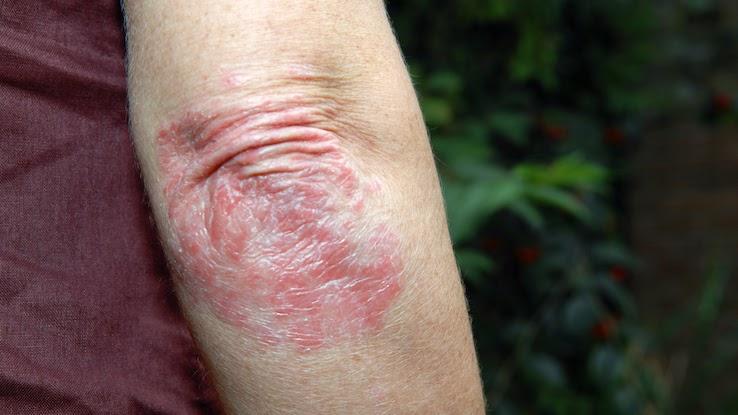
There are several subtypes of psoriasis: plaque psoriasis, guttate psoriasis, inverse psoriasis, nail psoriasis, erythrodermic psoriasis, pustular psoriasis and psoriatic arthritis. Each subtype varies in presentation and severity. Additionally, the severity of this condition may vary greatly from person to person. A dermatologist can accurately identify which subtype of psoriasis you have and ensure you receive the most appropriate treatment for it.
Plaque psoriasis is the most common form of psoriasis. It causes thick, raised patches of skin known as “plaques” to form. The plaques may be covered by scales, which appear as thin, silver-white pieces of skin. Plaques may differ in size and tend to occur in clusters. Most commonly, these plaques are found on the elbows, knees, scalp and lower back area.
Guttate psoriasis is characterized by small, reddish-pink bumps that arise suddenly and typically affect large areas of the torso, arms and legs. This type of psoriasis occurs more commonly in children and young adults following an infection such as strep throat. Guttate psoriasis tends to clear itself within several weeks or months and generally doesn’t require treatment. In some cases, the condition never returns; however, in others, it can flare again later in life.
Inverse psoriasis occurs most commonly in areas of skin-to-skin contact, such as the underarm region, genitals and area between the buttocks. It’s characterized by red, raw-appearing skin that’s sore and, in some cases, painful to the touch. This form of psoriasis is also known as intertriginous or flexural psoriasis.
Pustular psoriasis can be generalized (affecting large areas of the body) or localized (affecting only certain areas). Generalized pustular psoriasis is known to worsen quickly and can cause fever, chills, sweating, severe itching and muscle weakness. Localized pustular psoriasis affects the palms of the hands and the soles of the feet.
Erythrodermic psoriasis causes thick, red and inflamed patches that cover most of the skin. This type of psoriasis is considered a medical emergency and requires immediate treatment. People who develop erythrodermic psoriasis may already have another subtype of psoriasis. However, it’s particularly life-threatening because it can cause hypothermia by preventing skin from retaining warmth. Other symptoms include body chills, fever, tachycardia (fast pulse), severe itching, muscle weakness and skin that appears burned due to the extent of the inflammation.
Nail psoriasis often accompanies psoriasis in other regions of the body. It’s estimated that half of people with plaque psoriasis see nail symptoms, such as small dents in the nail, discoloration beneath the nail, nail lifting or brittle and rough nails.
Psoriasis can also affect a person’s joints in a condition that’s known as psoriatic arthritis. This form of psoriasis occurs most commonly alongside severe skin psoriasis. It’s characterized by joint pain, swelling around the joints (particularly the ankle and heel areas) and stiffness that feels worse in the morning.
Signs and Symptoms of Psoriasis

Symptoms of psoriasis vary by subtype and may present in many ways. They may commonly look like:
- Thickened areas of dry skin that appear red or pink
- Itchy, flaky or scaly areas
- Small, reddish-pink bumps
- Clusters of thickened, rash-like patches on the elbows, knees, ears or scalp
- Flaky skin on the scalp
- Nail crumbling or discoloration
More than one area of the body can develop symptoms at the same time. These symptoms can develop slowly or suddenly. Scratching or aggravating the skin may worsen symptoms of irritation.
When outbreaks occur, they tend to vary in severity. Rashes may appear on a person’s back, buttocks, arms, legs, underarms, stomach, genital area, face or joints. Headache, fever, chills and extreme pain might accompany the rash(es). Primary and accompanying symptoms may vary from person to person. Someone who has had a psoriasis flare in the past may be able to predict when another flare is likely to occur due to their experience with the symptoms.
Typically, psoriasis cycles through flare-ups and periods of remission that can last anywhere from days to months. Some cases are severe, while others are subtle. In some cases, the rashes clear on their own, leaving no residual scarring behind. In some more severe cases, however, the condition may recur throughout a person’s lifetime.
Sometimes people confuse psoriasis with allergic reactions, other rashes or sexually transmitted diseases, but a dermatologist can help rule out these other conditions. For the most part, people with psoriasis will experience regular and unpredictable flare-ups that are followed by periods of remission.
Symptoms of psoriasis often start in a person’s late teens to mid-twenties. Even with treatment, it’s expected that people with psoriasis will have flare-ups throughout their lives.
Related Conditions and Complications

There are several conditions related to and associated with psoriasis.
Autoimmune disease
Studies have shown that people with one form of an autoimmune disease are likely to be susceptible to developing another. For instance, both ulcerative colitis and Crohn’s disease are more common in people with psoriasis compared to those without this specific skin condition.
Cardiovascular disease
People with psoriasis may be at an increased risk of developing cardiovascular disease. This may be due to the fact that people with psoriasis have a higher incidence of obesity, diabetes and hypertension compared to the general population.
Certain forms of cancer
Research has demonstrated that, in a group of 2,700 patients over the age of 65, patients with psoriasis had a three-fold increased risk of developing lymphoma than the general population. There’s also some evidence that caucasian individuals who have undergone multiple ultraviolet (UV) light treatments for psoriasis are at an increased risk of developing melanoma (skin cancer).
Depression
Psoriasis is associated with an increased prevalence of depression and other mood disorders. Many people with psoriasis report feeling low self-esteem and a heavy psychological burden due to their condition, which can make them feel isolated or alone. In some cases, these depressive symptoms can lead to suicidal ideations or thoughts. If you or someone you know is in immediate danger or having suicidal thoughts, call the National Suicide Prevention Lifeline (1-800-273-8255).
Causes and Triggers of Psoriasis

While medical experts don’t know the exact cause of psoriasis, they do know that the condition has immune and genetic components. The disorder is believed to be an autoimmune condition that’s influenced by a genetic predisposition. Some scientists believe that psoriasis occurs when skin cells grow too rapidly. Others believe that symptoms occur when immune cells release inflammatory signals, leading to the characteristic skin irritation seen in psoriasis.
Flare-ups are relatively unpredictable, and there may be no discernable environmental factors that trigger these flares. Once a person has their first outbreak, they’re likely to develop another. While it is difficult to predict a flare-up, there are certain environmental, dietary and behavioral factors that can potentially lead to or exacerbate psoriasis rashes. Many people with psoriasis experience flare-ups while undergoing periods of extreme stress. Others develop psoriasis after too much or too little sun exposure.
Certain medications, topical creams, makeup and hair products can increase the likelihood of a flare-up. In addition, those who smoke cigarettes, have diabetes or have hypertension are also at an increased risk of developing psoriasis. Some people find that they tend to have more frequent flare-ups when their skin is dry rather than moisturized.
Many people who develop psoriasis have a family history of the condition, indicating a strong genetic component. Unfortunately, there are no tests that can indicate whether you will develop psoriasis in your lifetime. Documenting your behaviors can help determine what your personal triggers may be for a psoriasis flare-up.
Diagnosing Psoriasis

Psoriasis is typically diagnosed visually by a skin specialist or dermatologist. Your dermatologist may use an evaluation known as the Psoriasis Area and Severity Index (PASI) to measure the overall severity of your condition. Blood and urine tests may be required to rule out other conditions. It is recommended you examine your own skin regularly to notice any changes or persistent skin issues.
Visual Examination
There are no lab tests or blood tests available to confirm or deny the presence of psoriasis. Instead, a doctor must examine the skin and nails closely, sometimes analyzing the skin under a microscope. A primary care physician may be able to diagnose psoriasis. However, your physician may choose to refer you to a dermatologist or other specialist for a more precise diagnosis.
Skin Biopsy
Your physician may take a small sample of skin from an affected area to rule out other possible skin conditions, sexually transmitted diseases or infections. A skin biopsy generally does not require any form of pain management other than a local anesthetic. It can usually be done in an outpatient setting.
It’s important to tell your physician if you’re taking any medications prior to having a skin biopsy, as certain medications can change the appearance of your skin under a microscope. You may also undergo an allergy test to determine whether your rash is the result of an allergic reaction to a food, plant, animal or another kind of common environmental trigger.
Laboratory Testing
Psoriasis cannot be confirmed by a blood or urine test. However, a physician may order lab work to rule out other possible skin conditions, rashes or sexually transmitted diseases.
Psoriatic Arthritis
People with psoriatic arthritis usually experience joint swelling, pain and stiffness. Your physician may order a blood test to detect rheumatoid factor (RF), which indicates the presence of rheumatoid arthritis. This blood test may help your physician rule out other possible causes of your symptoms.
Imaging
Your physician may order an X-ray if you’re demonstrating symptoms of arthritis such as joint pain and stiffness. An X-ray can help determine if long-term damage has occurred to your bones due to your condition. The imaging alone cannot differentiate between psoriatic arthritis and other forms of arthritis, but it can help your physician build a complete picture of your condition.
Misdiagnosis
Psoriasis may be misdiagnosed due to its resemblance to conditions like acne, arthritis and sexually transmitted diseases. The condition may go undetected until symptoms become present. Because symptoms vary greatly from person to person, it can be difficult to determine a definitive list of psoriasis indicators. If you suspect you have psoriasis, you should visit a dermatologist or skin specialist.
Psoriasis Flare-ups, Remission and Treatments
While there is no cure for psoriasis, several treatments can help alleviate your symptoms. Treatments are based on the severity and location of a person’s rashes. A physician may prescribe a combination of topical creams, oral medications, biologics (injections) and ultraviolet radiation treatments.
What works for some people might not work well for others. If you’re diagnosed with psoriasis, it may take some time for your physician to develop a treatment strategy that offers you relief, and your physician may try out different treatments in steps so as to not overwhelm your body. Most providers begin with topical creams or treatments that are applied directly to the skin. Then, they move to more invasive treatments such as oral medications or phototherapy (UV treatment).
If the disease is mild and affects only a small area of skin, topical creams, moisturizers and sprays may be effective. For some people, the flare-ups may be more severe on some areas of the skin than others. Your physician may recommend topical or injected steroids for effective, localized treatment. Hydrocortisone is a commonly prescribed cream and injection that helps relieve itching, burning and swelling.
More severe cases of psoriasis may benefit from the use of biologics. These are medications that target certain components of the immune system. The use of light with phototherapy may also lessen symptoms of moderate psoriasis. If psoriasis progresses to a life-threatening stage, as can happen with pustular or erythrodermic psoriasis, surgical intervention may be necessary to prevent further complications such as organ failure.
Resource Links:
https://www.aad.org/public/diseases/psoriasis/what/symptoms
https://www.cdc.gov/psoriasis/index.htm
https://my.clevelandclinic.org/health/diseases/6866-psoriasis





